Acquired and infectious disease is a major health issue and can affect any member of the community regardless of race, color or sexual habits. However some groups are more at risk than others. Each year in the United States, as many as 50,000 people become infected with HIV, and nearly 13,000 people with AIDS die annually. In 2018, an estimated 50,300 new HCV (Hepatitis C Viral) infections occurred in the United States. Between 2010 and 2018, the reported number of acute HCV infections quadrupled. High rates of new infections were predominantly among young adults aged 20-29 years and aged 30-39 years.
Source: CDC HHS.gov U.S. Department of Health & Human Services
HCV infection is common among people with HIV who also inject drugs. Nearly 75% of people living with HIV who report a history of injection drug use are co-infected with HCV. All people who are diagnosed with HIV are recommended to be tested for HCV at least once. People living with HIV are at greater risk for complications and death from HCV infection. Fortunately, direct acting antivirals that are used to treat HCV work equally well in people with and without HIV infection.
The HIV problem
Of the approximately 1.2 million people living with HIV in the United States, CDC estimates nearly one in eight (more than 161,000 people) do not know they are infected. Because many new infections are transmitted by people who do not know they are infected, undiagnosed infection remains a significant factor fueling the HIV epidemic.
HIV testing has never been quicker or easier than it is today, and more people have been tested than ever before. But fear and misperceptions can still keep people from finding out their HIV status:
- Many people, even those who engage in high-risk behavior, do not get tested because they do not believe they are at risk for HIV infection.
- Others misunderstand the testing process, not realizing that rapid HIV tests can be done with a simple cheek swab or finger prick and provide results in as little as 20 minutes.
- Some are concerned that other people will find out that they have tested positive (or that they sought testing at all), although testing is completely confidential.
- Some may avoid testing simply because they are afraid their test will be positive.
Today, more than half of American adults have not yet been tested.
Prevention Challenges
- Too few people with HIV are aware of their infection
- Many people with HIV do not receive ongoing treatment
- Diverse populations need equal access to prevention information and tools
- Disparities in HIV rates are fueled by social and economic inequities
- Limited resources for HIV prevention
- Many Americans have become complacent about HIV
Percentage of people who have ever been tested, overall and by population, since 2010
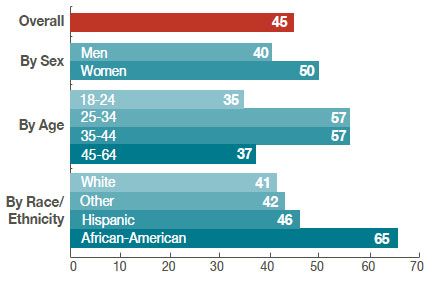
Many people with HIV do not receive ongoing treatment
Ensuring that people living with HIV receive ongoing care and treatment is one of the most effective ways to protect their health and prevent the further spread of HIV. Treating people with HIV lowers the amount of virus in their body and can dramatically reduce their risk of transmitting HIV to others. Of those living with HIV, just 40 percent receive regular medical care, and only 30 percent are successfully keeping their virus under control through treatment.
Diverse populations need equal access to prevention information and tools
Prevention programs must serve a diverse population that includes gay and bisexual men of all races and ethnicities – particularly those who are young, transgender women, and African Americans and Latinos – and help provide those populations with equal access to accurate prevention information and effective prevention tools. With more people than ever before living with HIV, it has also become increasingly important for prevention programs to address the needs of HIV-infected people and their partners.
Disparities in HIV rates are fueled by social & economic inequities
A wide range of complex social and economic factors drive the HIV epidemic and place African Americans and Latinos at greater risk for this disease. Many of the contextual factors that increase risk for other diseases (such as heart disease and diabetes) also fuel the spread of HIV within these communities:
High community rates of HIV: Because the burden of HIV is greater in some communities, African Americans and Latinos are at increased risk of being exposed to HIV infection with each sexual encounter. Therefore, even with similar levels of individual risk behaviors, African Americans and Latinos are at higher risk of infection than other races and ethnicities.
Poor access to health care: Having health insurance can enable a person to more easily access HIV care and treatment – but nearly 20 percent of African Americans and 30 percent of Latinos lack consistent health insurance, compared with 11 percent of whites.
Low socioeconomic status: CDC research shows that those who cannot afford the basics in life may end up in circumstances that increase their HIV risk. Census data indicate that in the United States poverty is not evenly distributed – nearly a quarter of African American and Latino families live in poverty (compared to 10 percent of white families).
Limited resources for HIV prevention
Today, the need to do more with existing resources is greater than ever. To achieve a higher level of impact with every federal prevention dollar, CDC is pursuing a High-Impact Prevention approach that works to match cost-effective, scalable interventions to heavily affected populations and geographic settings to maximize reductions in HIV incidence.
Many Americans have become complacent about HIV
Too many Americans no longer view HIV as a serious concern. A recent survey by the Kaiser Family Foundation found that the percentage of Americans who rank HIV as a major health problem is substantially lower than it was a decade ago. Even more troubling are studies showing that among some of the populations with the highest rates of infection (including gay and bisexual men and African Americans), many people do not recognize their risk, or they believe HIV is no longer a serious health threat.
Each new generation needs to be reminded of the still-serious nature of HIV and the importance of prevention. More than three decades after CDC reported the first cases of AIDS, the sense of national crisis may have waned – but our resolve cannot.
The Hepatitis C Problem
There is no vaccine for hepatitis C. The best way to prevent hepatitis C is by avoiding behaviors that can spread the disease, especially injecting drugs. Getting tested for hepatitis C is important, because treatments can cure most people with hepatitis C in 8 to 12 weeks.
- Hepatitis C is a liver infection caused by the hepatitis C virus (HCV). Hepatitis C is spread through contact with blood from an infected person.
- For some people, hepatitis C is a short-term illness, but for more than half of people who become infected with the hepatitis C virus, it becomes a long-term, chronic infection.
- Chronic hepatitis C can result in serious, even life-threatening health problems like cirrhosis and liver cancer.
- People with chronic hepatitis C can often have no symptoms and don’t feel sick. When symptoms appear, they often are a sign of advanced liver disease.
- About 40% of people with chronic hepatitis C are unaware of their infection. The only way to find out if you have an HCV infection is to get tested through a simple blood test.
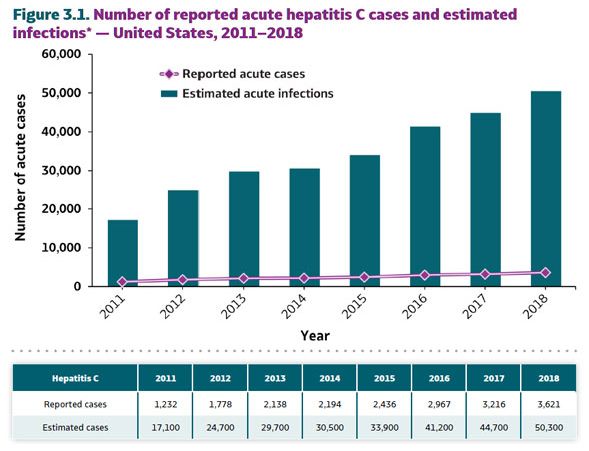
Source: CDC, National Notifiable Diseases Surveillance System.
* The number of estimated viral hepatitis infections was determined by multiplying the number of reported cases by a factor that adjusted for under-ascertainment and under-reporting(7). The 95% bootstrap confidence intervals for the estimated number of infections are shown in the Appendix.
Large section of the population is a risk from Hepatitis C
- People with HIV
- People who ever injected drugs and shared needles, syringes, or other drug preparation equipment, including those who injected once or a few times many years ago
- People with selected medical conditions, including:
- People who ever received maintenance hemodialysis
- People with persistently abnormal ALT levels
- Prior recipients of transfusions or organ transplants, including:
- People who received clotting factor concentrates produced before 1987
- People who received a transfusion of blood or blood components before July 1992
- People who received an organ transplant before July 1992
- People who were notified that they received blood from a donor who later tested positive for HCV infection
- Healthcare, emergency medical, and public safety personnel after needle sticks, sharps, or mucosal exposures to HCV-positive blood
- Children born to mothers with HCV infection
- Routine periodic testing for people with ongoing risk factors, while risk factors persist:
- People who currently inject drugs and share needles, syringes, or other drug preparation equipment
- People with selected medical conditions, including:
- People who ever received maintenance hemodialysis
To receive help for you or your community, call our outreach team

